Introduction
No-shows have long been considered one of the biggest operational challenges in clinics across the United States and Canada.
Missed appointments lead to:
- Lost revenue
- Underutilized staff
- Disrupted schedules
But are no-shows truly the root problem?
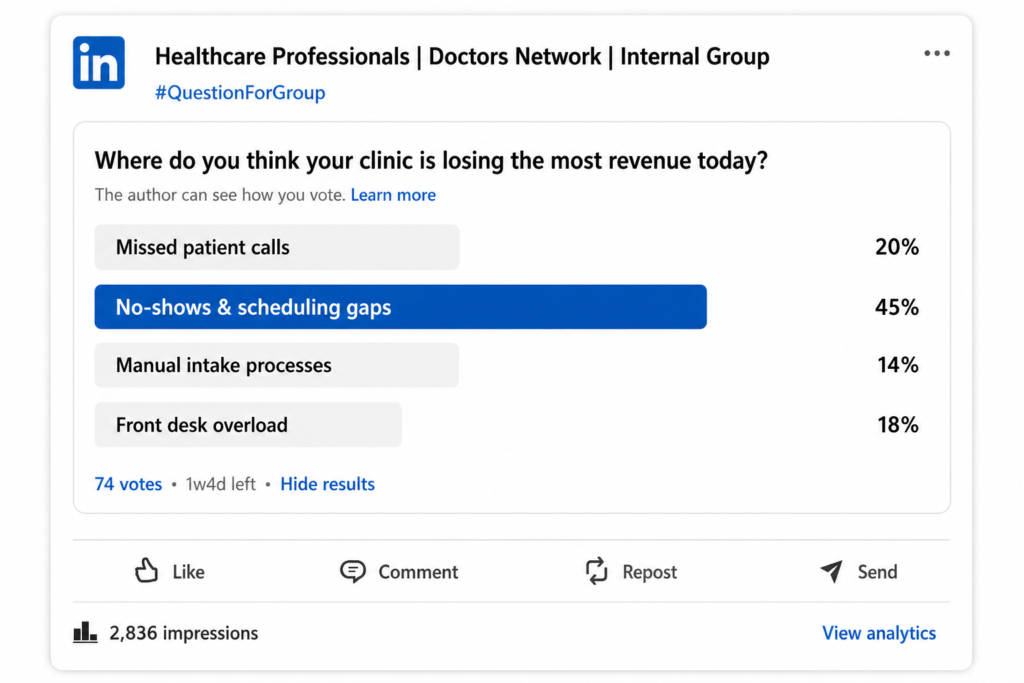
In a recent poll conducted among healthcare professionals, 45% of respondents identified “no-shows and scheduling gaps” as the biggest source of revenue loss.
At first glance, this seems accurate.
However, when you look deeper into the patient journey, a different picture emerges.
No-shows may not be the problem. They may simply be the final symptom of earlier operational breakdowns. Many modern applications of AI in healthcare now focus on improving operational efficiency and patient communication.
Table of Contents
What Healthcare Professionals Are Saying
In a recent LinkedIn poll among healthcare professionals, 45% of respondents identified “no-shows and scheduling gaps” as the biggest source of clinic revenue loss.
The poll included responses from:
- Physicians
- Healthcare administrators
- Clinical operations professionals
- Front desk and billing specialists
This highlights how strongly healthcare organizations associate operational inefficiencies with financial performance.
The Visibility Bias: Why No-Shows Get the Blame
No-shows are easy to track.
Clinic systems clearly show:
- Missed appointments
- Empty time slots
- Revenue gaps
Because these metrics are visible, they naturally become the focus of improvement strategies.
Most clinics respond with:
- Appointment reminders
- SMS confirmations
- Follow-up calls
While these tactics help, they address only the end of the patient journey.
What they often miss is what happens before the appointment is even confirmed.
What Happens Before a No-Show
From an operational perspective, patient drop-offs begin much earlier.
Across clinics in North America, several recurring friction points exist.
1. Limited Access to the Clinic
Many patients still rely on phone calls to book appointments.
Common challenges include:
- Calls going unanswered during peak hours
- No response after clinic hours
- Long hold times
In many cases, the patient never books at all.
This loss is rarely tracked, but it directly impacts clinic revenue.
2. Scheduling Friction
Even when calls are answered, the booking process can be inefficient:
- Back-and-forth coordination
- Limited visibility into appointment availability
- Manual scheduling workflows
Patients may abandon the process midway or choose another provider.
In competitive healthcare markets across the US and Canada, convenience plays a major role in patient decisions.
3. Inefficient Patient Intake
Traditional intake processes often involve:
- Paper forms
- Repetitive information entry
- Delays in verification and onboarding
This increases friction before the visit even begins.
Patients today expect faster and more convenient digital experiences.
4. Front Desk Capacity Constraints
Front desk teams manage multiple responsibilities simultaneously:
- Incoming calls
- Walk-ins
- Documentation
- Coordination with clinical staff
This often leads to:
- Delayed responses
- Missed interactions
- Inconsistent patient experience
Over time, this affects both patient satisfaction and operational efficiency.
The Real Problem: Patient Access, Not Attendance
When viewed holistically, the pattern becomes clear.
No-shows are not the root problem. They are a downstream outcome of access and workflow inefficiencies.
Patients do not simply fail to show up. Many:
- Never complete the booking process
- Drop off during scheduling
- Lose engagement before the visit
By the time a no-show appears in the system, the actual issue has already occurred.
Why Clinics Misdiagnose the Issue
Many clinics focus on improving:
- Attendance rates
- Reminder systems
- Confirmation workflows
While these are important, they operate too late in the patient journey.
The larger opportunity lies in improving:
- Accessibility
- Ease of booking
- Speed of communication
- Intake experience
The Role of AI in Improving Patient Flow
Across the United States and Canada, healthcare organizations are increasingly exploring AI to reduce operational friction and improve patient access. Rather than focusing only on reducing no-shows, many clinics are now looking at how AI can improve the entire patient journey — from the first patient interaction to post-visit communication. Similar operational improvements are already visible through various applications of AI in hospitals.
Here are some of the key ways AI is being used in clinic operations today
1. 24/7 Patient Communication
One of the biggest operational challenges for clinics is limited availability outside working hours. Many patients try to contact clinics during evenings, weekends, or busy periods when front desk teams may not be able to respond quickly.
AI-powered communication systems can help clinics manage:
- Appointment inquiries
- Basic patient questions
- Follow-up requests
- Rescheduling requests
This allows patients to receive faster responses without waiting for business hours. Improving response times can help clinics reduce patient frustration and improve booking conversion rates.
In highly competitive healthcare markets, convenience and accessibility are becoming major factors in patient retention.
2. Automated Scheduling
Traditional appointment scheduling often depends heavily on manual coordination between patients and administrative staff. This can create delays, long call times, and scheduling inefficiencies.
AI-assisted scheduling systems can help streamline this process by:
- Offering real-time appointment availability
- Reducing back-and-forth communication
- Automatically confirming appointments
- Managing rescheduling workflows
Faster scheduling experiences improve patient convenience while reducing workload on front desk teams.
For clinics managing high patient volumes, scheduling automation can also improve operational consistency and reduce administrative bottlenecks.
3. Digital Patient Intake
Patient intake is one of the most time-consuming administrative processes in healthcare. Many clinics still rely on paper forms or repetitive manual data collection during registration.
AI-enabled digital intake systems can help simplify onboarding by:
- Allowing patients to complete forms before arrival
- Collecting information digitally
- Reducing repetitive paperwork
- Improving data accuracy
This creates a smoother experience for both patients and staff. It can also help clinics reduce waiting room delays and improve overall workflow efficiency.
As patient expectations continue to evolve, digital-first intake experiences are becoming increasingly important across modern healthcare systems.
4. Administrative Workflow Support
Front desk teams handle a wide range of responsibilities throughout the day, including answering calls, managing schedules, processing patient information, and coordinating with clinical staff.
This high administrative burden can contribute to:
- Delayed responses
- Missed patient interactions
- Operational inconsistencies
- Staff burnout
AI systems can help support these workflows by automating repetitive tasks and improving coordination across administrative processes.
Rather than replacing staff, many healthcare organizations are using AI to reduce operational pressure and allow teams to focus on more patient-centered responsibilities.
Moving Beyond No-Show Management
This shift changes the conversation from simply managing missed appointments to improving the entire patient access system.
Instead of focusing only on reminder messages or attendance tracking, clinics are increasingly recognizing the importance of:
- Faster communication
- Easier booking experiences
- Reduced administrative friction
- Better patient engagement before the visit
Improving these areas can have a significant impact on both patient satisfaction and operational performance.
Why This Matters for Clinics in the US and Canada
Healthcare systems in North America continue to face pressure from:
- Rising patient expectations
- Staff shortages
- Administrative burden
- Growing competition among providers
Improving patient access is no longer optional.
It is directly connected to:
- Revenue performance
- Patient satisfaction
- Operational efficiency
While AI offers major workflow advantages, healthcare organizations must also consider the broader pros and cons of AI in healthcare.
Conclusion
No-shows are an important operational metric, but they should not be treated as the primary problem.
A more effective question for clinics is:
How many patients never made it to the schedule in the first place?
Understanding and improving this earlier stage of the patient journey can lead to better patient experiences, stronger operational efficiency, and improved financial outcomes.
FAQs
1. Why are no-shows a problem for clinics?
No-shows reduce clinic revenue, waste staff time, disrupt scheduling, and lower operational efficiency. They can also increase wait times for other patients seeking appointments.
2. What causes patient no-shows in healthcare?
Common causes include scheduling delays, unanswered calls, poor communication, long intake processes, transportation issues, and lack of patient engagement before appointments.
3. How can clinics reduce no-shows?
Clinics can reduce no-shows by improving patient communication, simplifying scheduling, automating reminders, streamlining intake processes, and reducing administrative friction.
4. How is AI used to improve patient scheduling?
AI can support automated scheduling, handle appointment requests 24/7, manage patient communication, and reduce delays caused by manual coordination.
5. Why is patient access important in healthcare?
Better patient access improves appointment conversion, patient satisfaction, operational efficiency, and overall clinic revenue by reducing drop-offs before booking.


0 Comments